Your Child’s First PT Evaluation: What to Expect
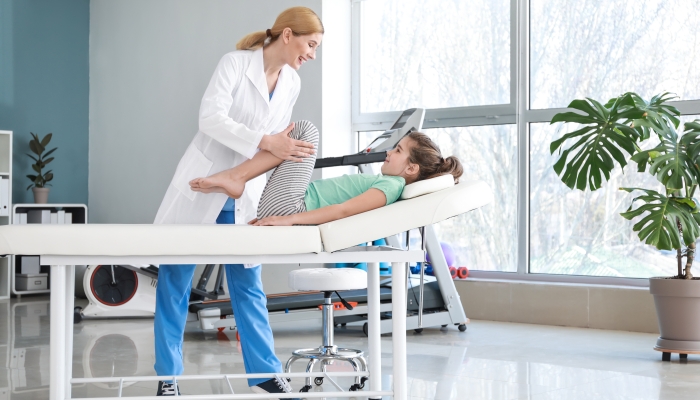
- An evaluation is the first appointment your child will have with their physical therapist.
- The physical therapist will take a detailed medical history and perform a physical exam.
- The initial physical therapy evaluation findings determine if PT is right for your child and helps the therapist create a treatment plan unique to your child’s needs.
- A child’s parent or guardian is expected to play an active role in during the child’s PT treatment.
A referral to physical therapy may seem overwhelming for you and your child—especially if your child already has many medical appointments!
Having a physical therapy evaluation does not need to be a source of further stress. Your child’s physical therapist is trained to provide insight and education about your child’s situation after carefully examining their clinical presentation.
Think of the physical therapy evaluation as an opportunity for you to learn more about your child’s diagnosis and to make your concerns known to a member of your child’s medical team. The one-on-one attention given in PT sessions enables you to develop a strong relationship with a medical provider that will help your child change and grow over time.
PT Evaluation: What Is It?
The first appointment with a physical therapist is called an initial evaluation. This appointment allows the physical therapist to learn about your child’s case and perform a physical examination. Then the physical therapist will use your child’s medical history and clinical presentation to decide if physical therapy is right for them.
If your child is referred to physical therapy, they likely have some difficulty with gross motor skills like standing, jumping, walking, or running. Their trouble may be the result of injury, surgery, or congenital diagnoses. Physical therapists also address developmental delay, balance, coordination, pain, and joint range of motion, though that is not a full list.
Pediatric physical therapists may treat your child in an outpatient clinic, a hospital, a school or daycare, your home, or a specialty clinic (e.g., the NICU, a burn unit, or a hand clinic). Physical therapy is different from occupational, recreational, and speech therapy, though the different allied health disciplines often complement each other.
The physical therapist may feel that your child does not need skilled services at the time of the evaluation. They may also feel that your child needs the services of other therapists or physicians if your child’s case is complex. Your child’s case is rated as low, moderate, or high complexity based on a variety of factors.
After the initial physical therapy appointment, your child’s physical therapist creates a treatment plan that consists of goals, the number of visits, expected treatment duration, and a home exercise plan.
The treatment plan will be tailor-made for your child to meet their unique needs. This plan may change over time as the therapist sees how your child responds to their treatment sessions.

Things to Bring for Your Child’s PT Evaluation
Please bring the following documents and items to your child’s appointment:
- Yourself! It’s important that an adult parent or guardian is present to provide a medical history and answer any questions.
- Current insurance card. If this information changes, please update your child’s medical providers as soon as possible to avoid a gap in care!
- Any written prescriptions or instructions from your child’s physician that were not sent electronically or via fax. This includes surgical or wound care instructions if relevant to your child’s history.
- Documents or imaging if not sent electronically. For example, x-rays of fractures, spinal curves, or arthritic changes
- Bag or list of current medications.
- Clothes and shoes appropriate for exercise.
- Any equipment relevant to the evaluation. Is this appointment for an adaptive equipment evaluation? Do they need to learn to use crutches or a walker? Have they recently had surgery and are using a brace or other equipment?
What to Expect During Your Child’s Initial PT Evaluation?
When you arrive for your child’s physical therapy evaluation, you will first have to fill out paperwork, so plan to arrive early. This may include HIPAA (privacy), consent to treat, consent for release of medical information, and general intake forms. You must provide your child’s insurance card and possibly a photo ID of the responsible adult.
Your child’s physical therapist will then bring you back to the treatment areas to take a medical history and perform a physical assessment. Some therapists are comfortable taking a history while beginning to observe your child move around and play. Others may take notes on paper or their computer as you talk to include in their documentation.
Questions asked during the evaluation may include the following:
- Describe your child’s birth history.
- Describe your child’s medical history. Are they under a doctor’s care for any diagnoses?
- What surgeries has your child had and when and why did they occur?
- What medications is your child currently taking? Are they experiencing any side effects?
- When did this current problem begin?
- Is your child in pain? What is their pain level and how would they describe the pain? (The therapist may direct questions like these to your child if they are able to understand and answer appropriately.)
- Does your child need help to complete activities that their peers are able to do? How much help do you provide?
- Does your child use any adaptive equipment to help with mobility or activities of daily living?
- Has the doctor given your child any instructions or exercises to do at home?
- Has your child ever been to physical, occupational, or speech therapy?
- What are your concerns? Do you feel like your child is meeting their developmental milestones?
The physical therapist will also review your child’s body systems and may take their weight and height, blood pressure, heart rate, or listen to their lungs. This occurs less often in outpatient and school settings, but may be completed if your child has a history of cardiopulmonary disease.
The therapist will spend more time on some parts of the assessment than others. Physical assessments often include the following:
Observation
General: Standing and sitting posture, joint position and alignment, behavior, wellness (pallor, swelling, redness, alertness)
Infants: Early reflexes, gross motor milestones like rolling, reaching, crawling, sitting, head control, standing
Functional Mobility Status: The ability to independently walk, crawl, stand, run, or use adaptive equipment to access their environment
Play: Balance, coordination, ability to play with others, age-appropriate skills like jumping and throwing
Level of Assistance: How much help do you give your child and what does that look like?
Wounds: How is your child healing from surgery or trauma?
Range of Motion
Your child’s physical therapist will look at how easily your child’s joints move and how flexible their muscles are.
Strength
Your child’s therapist may look for asymmetries in strength, areas of significant weakness, and patterns of weakness to determine the source of musculoskeletal or neurological complaints.
Neurological Assessment
This includes assessing reflexes, muscle tone, balance, coordination, vision or other special senses.
Girth Measurement
Typically this is used to assess changes in swelling.
Special Tests
These are hands-on physical assessments designed to help determine the source of a physical ailment.
Standardized Assessment
A standardized assessment compares your child’s results to that of age-matched peers for things like gross motor skills, balance, mobility, endurance, and coordination
The physical exam gives the physical therapist specific measurements that will help them to set realistic goals and get visits approved by insurance. Without these measurements, it is hard for the therapist to quantify your child’s progress over time.
Be aware that some parts of the physical exam are hands-on. The therapist should inform you and your child what will be done and perform the exam without causing unreasonable pain. Your therapist should also protect your child’s modesty if any clothing needs to be removed to assess a specific body part.
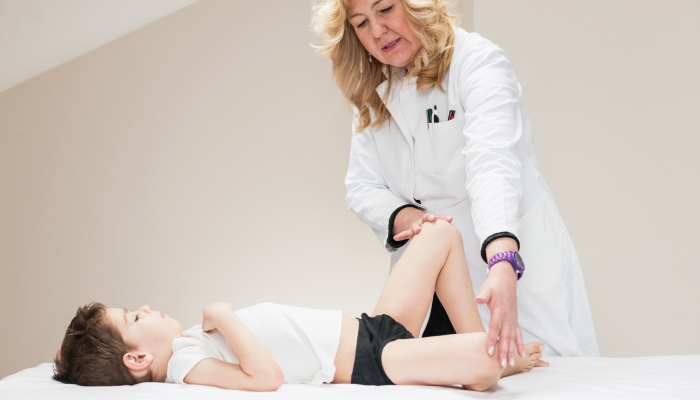
How to Prepare for Your Child’s First PT Evaluation
Your child should arrive at their appointment wearing comfortable clothes to move around in. Appropriate footwear is also recommended (i.e., tennis shoes). Children are discouraged from wearing sandals or boots unless there is a medical reason to do so (e.g., excessive swelling of the feet or ankle, using a walking boot, etc).
You can make your child more comfortable by telling them that their therapist will watch them move and measure those movements.
If a child becomes distressed during a session, the therapist take a break for free play and return to the activity later. You may bring toys or comfort items to soothe your child or help them feel at ease. If your child is an infant, having diapers and milk on hand will keep them comfortable.
As the parent, you should be present during the evaluation to provide information about your child’s medical history. As therapy progresses, you will continue to be an active member of the “team” by giving updates, telling the therapist your concerns, and doing exercises at home with your child. You know your child best and can give the therapist great insight into how best to help your child.
Please feel comfortable asking your child’s therapist anything during an initial evaluation. Be sure to find out if the therapist thinks your child should continue PT, how often visits will occur, and if they have any instructions or exercises to work on while waiting for insurance approval. You may ask questions at any time while your child is in physical therapy.
How Long Does a PT Evaluation Last?
Though treatment sessions have a predetermined length, the time to complete a physical therapy evaluation may vary. Most initial evaluations will take approximately an hour.
Therapy evaluations may take more or less time depending on your child’s tolerance and the complexity of their case. Additionally, the evaluation may take longer if more than one discipline is present (like speech or occupational therapy).
If physical therapy is right for your child, the therapist will write a note detailing the initial assessment. The therapist sends the note to your child’s physician to sign and then to the insurance company. Before treatment sessions can begin, the therapist’s office must first receive the doctor’s signature and insurance approval.
This process may take weeks. If the therapist has difficulty getting approval from your child’s approval, they may request more information to support your child’s case. Difficulty with insurance approval is more common with re-evaluations and large adaptive equipment orders than with the initial evaluation.
FAQs
Will insurance cover the cost of a PT evaluation?
The cost of a PT evaluation varies widely across insurances. If your child has Medicaid, copays and additional charges are likely to be low and may even be fully covered. Private insurance typically has a faster approval process, but may cost more and limit the number of therapy visits in a calendar year.
It’s best to contact your insurance company directly if your child is referred for physical therapy.
What is the difference between a physical therapy examination and a physical therapy evaluation?
A PT evaluation is a formal appointment to get insurance approval for more visits. Evaluations happen before the first treatment session and then once or twice a year thereafter depending on insurance requirements.
A PT examination may occur at any time during an evaluation or treatment session. During an exam, physical therapists gather data about a patient to inform their clinical decision-making.
These examinations may occur because a therapist notices a change in your child, must update the insurance company about your child’s progress toward their goals, or if your child has a change in medical status or new concern. The therapist may take detailed notes when performing an examination like they would during an evaluation.

The information WonderBaby provides is not intended to be, and does not constitute, medical or other health advice or diagnosis and should not be used as such. Always consult with a qualified medical professional about your specific circumstances.
Related Posts

Eye Conditions and Syndromes, Visual Impairment
Neuralink Announces Plans to Restore Sight to the Blind with Brain Chip
Elon Musk’s company Neuralink has announced plans to begin human trials of its new “Blindsight” brain chip by the end of 2025.

Special Needs
5 Spring Cleaning Tips for Families of Children with Disabilities
Spring cleaning is an opportunity to create a more accessible, organized, and supportive space for your child with disabilities. Declutter, deep clean, and refresh!

Visual Impairment
The Gift of Understanding: How a Young Child Helps His Blind Father Navigate Life
When a parent is blind, it’s natural for people to wonder how their sighted child will adapt. Will they struggle to understand their parent’s needs? Will they feel burdened by...